 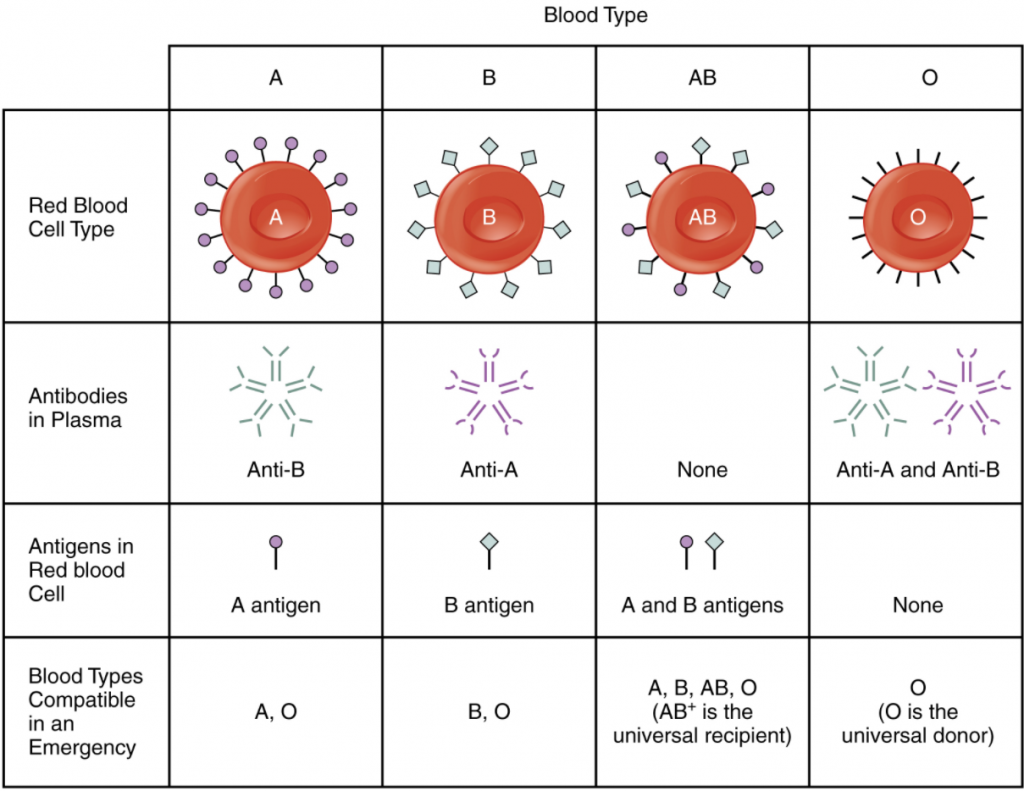 
Importantly, HLA antibody levels can change following events such as blood transfusions, miscarriages, minor surgeries (including dental work or fistula replacement) or severe infections, so you should communicate these events to your transplant team. If a patient has HLA antibodies in their blood, they are considered HLA “sensitized” and it is best to find a donor with HLA types that avoid the HLA antibodies in the patient’s blood. HLA antibodies can be harmful to the transplanted organ, and they can increase or decrease over time so they must be measured while waiting for a transplant, immediately before a transplant surgery, and following transplantation. The second blood test measures antibodies to HLA this test is done for the patient only and is repeated frequently (sometimes monthly but less often dependent upon the transplant program policy). The 2 steps above can accurately determine your blood type. Type O blood contains both types of antibodies. People with type B blood have anti-A antibodies. People with type A blood have anti-B antibodies. (This is known as a zero mismatch.) It is possible for all markers to match, even with an unrelated deceased donor organ, if the patient has a very common HLA type. The liquid part of your blood without cells (serum) is mixed with blood that is known to be type A and type B. The best match for the recipient is to have a full match. Because of the way chromosomes/DNA are inherited or passed down in a family, a parent and child would have at least a 50 percent chance of matching, siblings could have a zero to 100 percent match, and unrelated donors would be less likely to match at all. It is believed that the better the HLA match, the more successful the transplant will be over a longer period of time. Each person's tissues, except for identical twins, are usually different from everyone else's. Despite its reputation as a universal option, however, even O- blood may have antibodies that react with other types. 
In an emergency or if your life is in danger, medical personnel will most commonly administer O- blood. IMPORTANT: The ordering physician must sign a waiver if the urgency of the situation requires the release of uncrossmatched (group O) RBC units from the Blood Bank.The first blood test is to determine the tissue (HLA) type of the patient and the potential donor to see how well they match. Long considered a universal blood type, O- blood tends to be compatible with all other standard blood types. Potential who require urgent or continued RBC transfusions. Transfuse Rh+ RBCs to Rh- males as well as females of non-childbearing Should or must receive only this type, it is common practice to Maintain an adequate supply of O- RBCs for these and other patients who To avoid the possibility of alloimmunization. Whenever possible group 0- RBCs should be used forįemales of childbearing potential (generally women < 55 years of age) Many hospitals in the United States have a limited supply of Response requires approximately 3 to 4 months to develop and the patient The probability of forming anti-D after transfusion Positive or Rh negative RBCs, particularly in an emergency situation.Īn Rh- individual may make anti-D only if exposed to theĭ-antigen via transfusion with Rh+ blood or platelets, or if pregnant Such individuals could be safely transfused with either Rh Individuals who have not been exposed to the Rh antigen will not makeĪnti-D. Under normal circumstances, Rh negative (Rh-) Unlike the ABO system, there are no naturally occurring (pre-formed) antibodies to the "D" antigen in the Rh system. The Rh system is immunologically different than the ABO system. As soon as the patient's ABO/Rh isĮstablished, the patient will be converted to type specific crossmatched Group, the safest course of action is to provide group O RBCs otherwiseĬonsidered uncrossmatched RBCs. 
When clinicalĬircumstances do not allow time for determination of the patient's ABO Significant amount of blood during this time. To perform, in certain critical situations a patient may lose a Although ABO group typing only requires 5-10 minutes ABO compatibility of Red Blood Cells (RBC) is fundamental to 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
